Why Didn't You Come Sooner? — A Zambian Mother, Living With HIV, Exposes Her Child to the Virus (CP in Zambia 2)
Correction Appended
Editor's note: The Christian Post was invited by World Vision Zambia to meet with locals who have been impacted by the organization's water, sanitation and hygiene program. This is the second of a series of articles on that trip, which took place March 22-28. Read part one: Sickness, Discomfort and Death: the Fate of Families and Children With No Access to Clean Water.

A woman, perhaps in her 30s, sat on the bench adjacent to the nurse's desk. Her child, 15 months old, sat tucked inside the colorful homemade sling strapped across her back and her left side. It was finally her turn to speak with the nurse. Her child's nearly-bare head bobbed from side to side as he peered wide-eyed around the 8x10 room at the narrowed eyes set in strange faces peering back at him. But the strangers could not hold his steady gaze, their eyes weighed down by the sadness and shock that gripped them after his mother had entered into the room.

There was anger, too, and frustration, expressed on the part of the nurse who sat at a desk that was sandwiched between the window on her left and the bench, occupied by the mother and her child, on her right.
The nurse's smooth, brown face appeared taut and her eyes betrayed her mood as she conversed with the woman in Tonga, one of Zambia's major languages. This was the Moyo ADP Health Center in southern Zambia and the nurse, 28-year-old Bertha Himaanga, did not seem at all pleased as she questioned the unidentified mother:
"When did you last visit the clinic?"
"Why didn't you come sooner?"
"Have you been taking your medicines?"
The child's mother was HIV-positive, and was supposed to be taking medicine. But she had not been doing so, although she had been breastfeeding the toddler — and exposing him, with every suck and swallow of milk he took, to the virus that kills thousands of Zambia's babies and children every year. The boy, whose name was not revealed, was having difficulty keeping down food, the woman told the nurse.
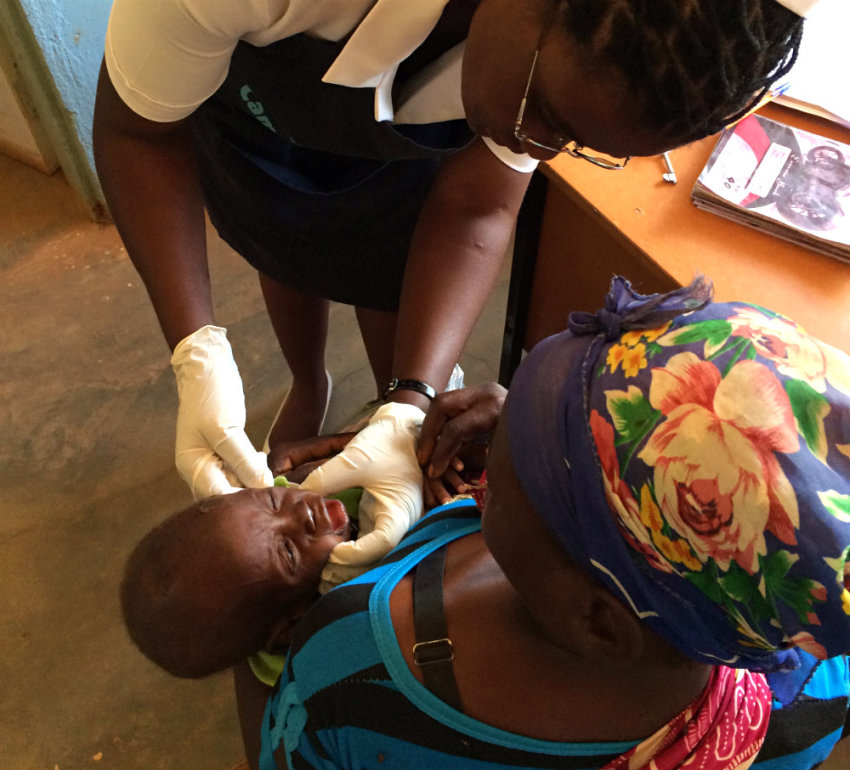
Himaanga, the only nurse among a staff of three on duty that day, rose from her chair, disappeared into an adjacent room, and seconds later reappeared wearing latex gloves. She approached the baby and gently pried open his mouth. The child squealed in discomfort.
Less than half a minute later Himaanga removed the gloves, disposed of them in a trash can, and sat back down at her desk. She opened a thin notebook, one that resembled the dozens of others piled on top of a second and nearby desk, and started writing on one of its pages.
The room was quiet, except for the sound of some observers, a part of a small group that was visiting the clinic that day, shuffling around the stone-floored room and taking photos. Hushed chatter and faint laughter from the other women waiting in line outside drifted into the room. Those among the visiting group who were not taking photos, instead studied the mother and her child.
There was a small wound on the baby's forehead that seemed too stubborn to heal. His face appeared slightly gaunt, and his head had tufts of brown hair in random places. Apart from the momentary intrusion from Nurse Himaanga, the child did not make a sound.
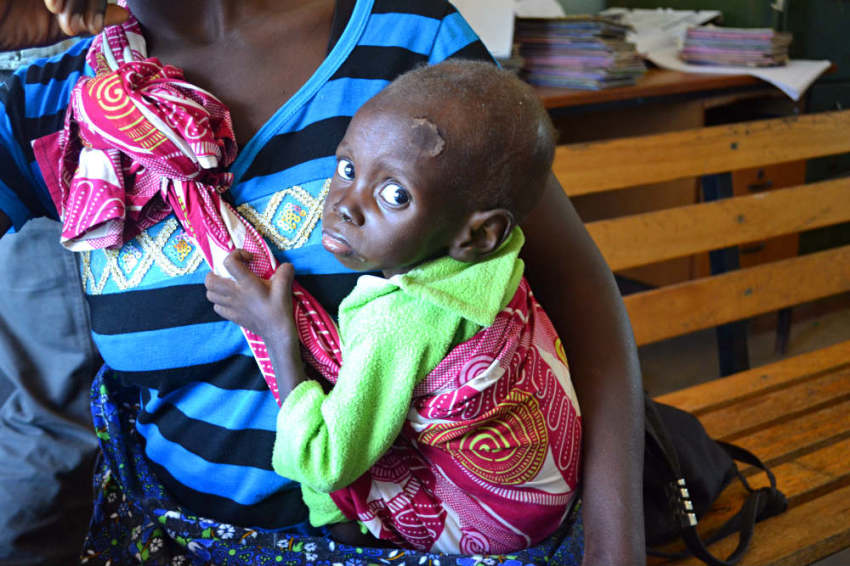
Although only a test could determine for certain whether or not the baby, born HIV-free, was now himself infected, those standing about the room, their curiosity overriding the compulsion to look away, suspected that it was already too late for the boy, present less than two years in the world. Afterward, Nurse Himaanga, who had shared during an earlier chat that she entered the profession because she "felt like (she) could help save people's lives," confessed that she also suspected that the child was infected.
Himaanga also told us, the small visiting group of journalists, a blogger and World Vision staff members, that the mother had lied to her three times when she was asked how often she had returned to the health center since giving birth to her child at the facility.
The mother, who had three other children at home, all HIV-free, had stayed away from the health center because "she's been busy," Himaanga told us, and her husband was not of much help.
In Zambia, where about 14.5 million people live, women's work at the home involves, among other things, cleaning, cooking, washing and — if she is among the 4.8 million living in the rural areas without a clean water source — walking miles, in some cases, to a dam or pond to fetch (unsanitary) water to do all of those chores. These are chores that could literally take a woman all day to do.
But this woman had not been taking her medicine. None among the observing group had asked what might have been the reason for that neglect.

The Moyo Health Center, the name of which means "heart" or "life," is a part of a local World Vision Area Development Program. World Vision began its work in Zambia in 1981, first directing its attention to three community programs in one district. By 1995, World Vision Zambia had introduced the Area Development Programs, or ADPs. These ADPs, currently numbering 39, spanning 29 districts and serving more than 2 million people, provide service and education in the areas of health, nutrition, livelihood security and economic development.



























